Why do we all need a colonoscopy at age 45? Is there anything else I can do?
Have you ever had this question asked of you before? I know I have. We at Ark Family Health want to keep you informed as to why testing is recommended, what options are available to you and how we can help you take care of yourself best. Preventative care is something we are very passionate about and we are able to provide you with this important portion of your health.
Colorectal cancer (CRC) is the second leading cause of cancer death in the United States. In 2016, an estimated 134,000 persons will be diagnosed with the disease, and about 49,000 will die from it. Colorectal cancer is most frequently diagnosed among adults aged 65 to 74 years.
Colorectal cancer develops in the large intestine (colon) or rectum. The primary goal of colon cancer screening is to prevent deaths from colon cancer. Screening tests can help identify cancers at an early and potentially curable stage. Screening can also prevent the development of cancer by identifying and treating precancerous abnormal growths that can be removed before they become malignant.
The US Preventive Services Task Force (USPSTF) issued new guidelines for CRC screening in 2016. They make a strong recommendation for screening, starting at age 45 years for AVERAGE-RISK adults, but do not give preference for any one of seven screening testing modalities over another. In addition, screening individuals 76-85 years old should be individualized (C recommendation) – The American Academy of Family Physicians’ (AAFP) 2016 Clinical Preventive Service Recommendation recommends only FIT, flexible sigmoidoscopy, or colonoscopy for average-risk CRC screening starting at age 45 years and continuing until age 75 years.
Is there more than just a colonoscopy?
The answer is yes, absolutely. The USPSTF guidelines support the following 7 screening options:
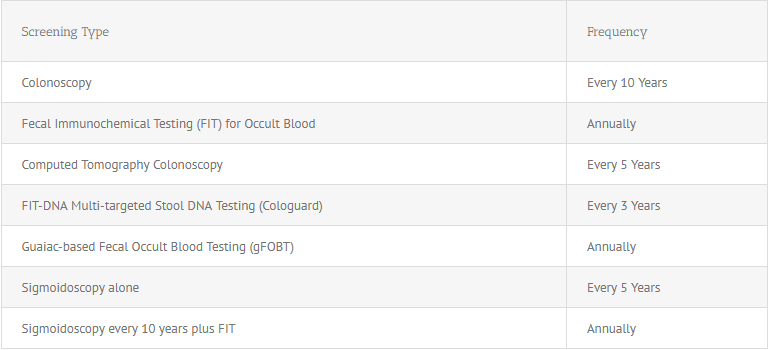
Let’s briefly take each one and break it down.
1. Colonoscopy
Definitive test for detection of advanced adenomas and CRC. The biggest advantage is it allows for diagnostic and therapeutic evaluation, with the ability for biopsy and/or excision of lesions in one single study. Disadvantages relate to the need for specialized equipment/specialists, cost (we have resources that estimate a colonoscopy ~$1200), need for vigorous bowel preparation, potential complications related to conscious sedation, and risks of the procedure itself, such as perforation and bleeding.
2. FIT testing annually
FIT is more expensive than guaiac-based test, but more convenient and has the potential to be more cost-effective if fewer colonoscopies are needed for follow-up. Studies have suggested that immunochemical tests, compared with stool guaiac tests, may have better performance characteristics for screening. Immunochemical-based stool testing is usually performed on a single stool sample, which is usually self-collected at home and processed in a laboratory; the quantitative versions of the test are processed using standardized automated analyzers. FIT does not require modification of diet or medications. Positive tests should be followed by colonoscopy. The hemoglobin in the sample can degrade and lower the test accuracy when exposed to high ambient temperatures; therefore, it is important to return the sample immediately and avoid mailing on high temperature days.
3. CT Colonography every 5 years
CT colonography (CTC) uses computers to construct images of the bowel mucosa in two and three dimensions. Advantages of CTC are that it is noninvasive, does not require anesthesia, visualizes the entire bowel, and detects large adenomas just about as well as optical colonoscopy. Disadvantages include: abnormal results need to be followed up by colonoscopy for excision and tissue diagnosis, flat adenomas that may have greater malignant potential than polypoid lesions are more likely to be missed on CTC than colonoscopy. There is always the radiation exposure risk. Extracolonic findings (outside the colon) from CTC lead to over-diagnosis (identifying disease that would not cause problems in a patient’s lifetime), the cost and risk of additional evaluations, and the worry associated with abnormal findings.
4. FIT DNA Testing (Cologuard) every 3 years
Stool DNA testing is available as part of a composite test, including an immunochemical assay (same as FIT), molecular assays for DNA (KRAS) mutations, and methylation biomarkers associated with colorectal neoplasia. Stool DNA testing has a higher single-application sensitivity and a lower specificity than FIT, but it is more expensive than FIT. Testing requires collection of a single bowel movement and is sent to a laboratory for processing.
5. gFOBT annually
A stool sample to detect hemoglobin, a sign of bleeding in the colon. Advantages include: No bowel preparation needed, Noninvasive, and easy and effective. Some disadvantages are: It is NOT a good test for polyp detection (polyps usually don’t bleed). You should avoid drugs such as aspirin and NSAIDs before collecting stool. Any positive testing requires further workup, usually with a colonoscopy, and some results are falsely positive. With guaiac testing, you collect two samples of stool from three consecutive bowel movements, which you apply to home collection cards. You mail the cards back to the health care provider.
6. Sigmoidoscopy alone every 5 years
Similar to a colonoscopy, the 60 cm flexible sigmoidoscope can identify only left-sided colon lesions, which are more common in men, whereas colon lesions (cancers or polyps) are more likely to be right-sided in women and would be missed. Advantages include: less onerous bowel preparation than for colonscopy or CTC, and procedure can be performed without sedation in office with the right equipment. Disadvantages are similar to colonoscopy, specifically perforation, although less than colonoscopy. Also, larger lesions aren’t able to be biopsied.
7. Sigmoidoscopy every 10 years plus FIT annually
A combination of the 2 has shown to be more effective than either by themselves.
WHY COLON CANCER SCREENING WORKS — Most colorectal cancers develop from precancerous polyps. Polyps are growths that arise in the lining of the colon and are visible when the bowel is examined by endoscopy (colonoscopy or sigmoidoscopy) or (CT) scan (CTC). There are two types of polyps: adenomatous and hyperplastic. Adenomatous polyps can become cancerous over time; this progression takes at least 10 years in most people.
Colon cancer screening tests work by detecting polyps or early stage cancers followed by removal of the abnormality. Regular screening for and removal of polyps reduces your risk of developing colorectal cancer (by up to 90 percent with colonoscopy). Early detection of cancers that are already present in the colon increases the chance of successful treatment and decreases the chance of dying as a result of the cancer.
Colon Cancer Risk Factors
- Family history of colorectal cancer – Having colorectal cancer in a family member increases your risk of cancer if the family member is a first-degree relative (a parent, brother or sister, or child), if several family members are affected, or if the cancers occurred at an early age (e.g., before age 45 years).
- Prior colorectal cancer or polyps – People who have previously had colorectal cancer have an increased risk of developing a new colorectal cancer. People who have had adenomatous polyps before the age of 60 years are also at increased risk for developing colorectal cancer. Screening recommendations for these groups are quite different and should be discussed with your physician.
- Increasing age – 90% of colorectal cancers occur in people older than 50 years of age. Risk increases with age throughout life.
- Lifestyle factors – Several lifestyle factors increase the risk of colorectal cancer, including:
- A diet high in fat and red or processed meat and low in fiber
- A sedentary lifestyle
- Cigarette smoking
- Alcohol use
- Obesity
- INFLAMMATORY BOWEL DISEASE – People with Crohn’s Disease or Ulcerative Colitis have an increased risk of colorectal cancer. The amount of increased risk depends upon the amount of inflamed colon and the duration of disease. The risk of colon cancer is not increased in people with irritable bowel disease.
Factors that may decrease risk — Aspirin, ibuprofen, and related non-steroidal anti-inflammatory medications may decrease the risk of developing colorectal cancer.
References:
- Levin B, Lieberman DA, McFarland B, et al. Screening and surveillance for the early detection of colorectal cancer and adenomatous polyps, 2008: a joint guideline from the American Cancer Society, the US Multi-Society Task Force on Colorectal Cancer, and the American College of Radiology. CA Cancer J Clin 2008; 58:130.
- Whitlock EP, Lin JS, Liles E, et al. Screening for colorectal cancer: a targeted, updated systematic review for the U.S. Preventive Services Task Force. Ann Intern Med 2008; 149:638.
- Atkin WS, Edwards R, Kralj-Hans I, et al. Once-only flexible sigmoidoscopy screening in prevention of colorectal cancer: a multicentre randomised controlled trial. Lancet 2010; 375:1624.
- Mandel JS, Bond JH, Church TR, et al. Reducing mortality from colorectal cancer by screening for fecal occult blood. Minnesota Colon Cancer Control Study. N Engl J Med 1993; 328:1365.
- Screening for Colorectal Cancer: US Preventive Services Task Force Recommendation Statement. US Preventive Services Task Force, Bibbins-Domingo K, Grossman DC, Curry SJ, Davidson KW, Epling JW Jr, García FA, Gillman MW, Harper DM, Kemper AR, Krist AH, Kurth AE, Landefeld CS, Mangione CM, Owens DK, Phillips WR, Phipps MG, Pignone MP, Siu AL. JAMA. 2016 Jun;315(23):2564-75.
- http://www.aafp.org/patient-care/clinical-recommendations/all/colorectal-cancer.html (Accessed on November 23, 2016)
- http://www.uptodate.com/contents/screening-for-colorectal-cancer-strategies-in-patients-at-average-risk?source=see_link#H13101193





